Venous Health & Wellness: Tips and Strategies to Improve Vascular Health and Prevent Vein Disease
Your veins play a crucial role in maintaining your overall health and well-being. They are responsible for transporting deoxygenated blood back to your heart, ensuring proper circulation throughout your body. When your venous system is healthy, you’re less likely to experience issues like varicose veins, deep vein thrombosis (DVT), or chronic venous insufficiency (CVI). While there are no guaranteed ways to prevent vein problems, you can take proactive measures and implement lifestyle changes to improve your vascular health and reduce the risk.
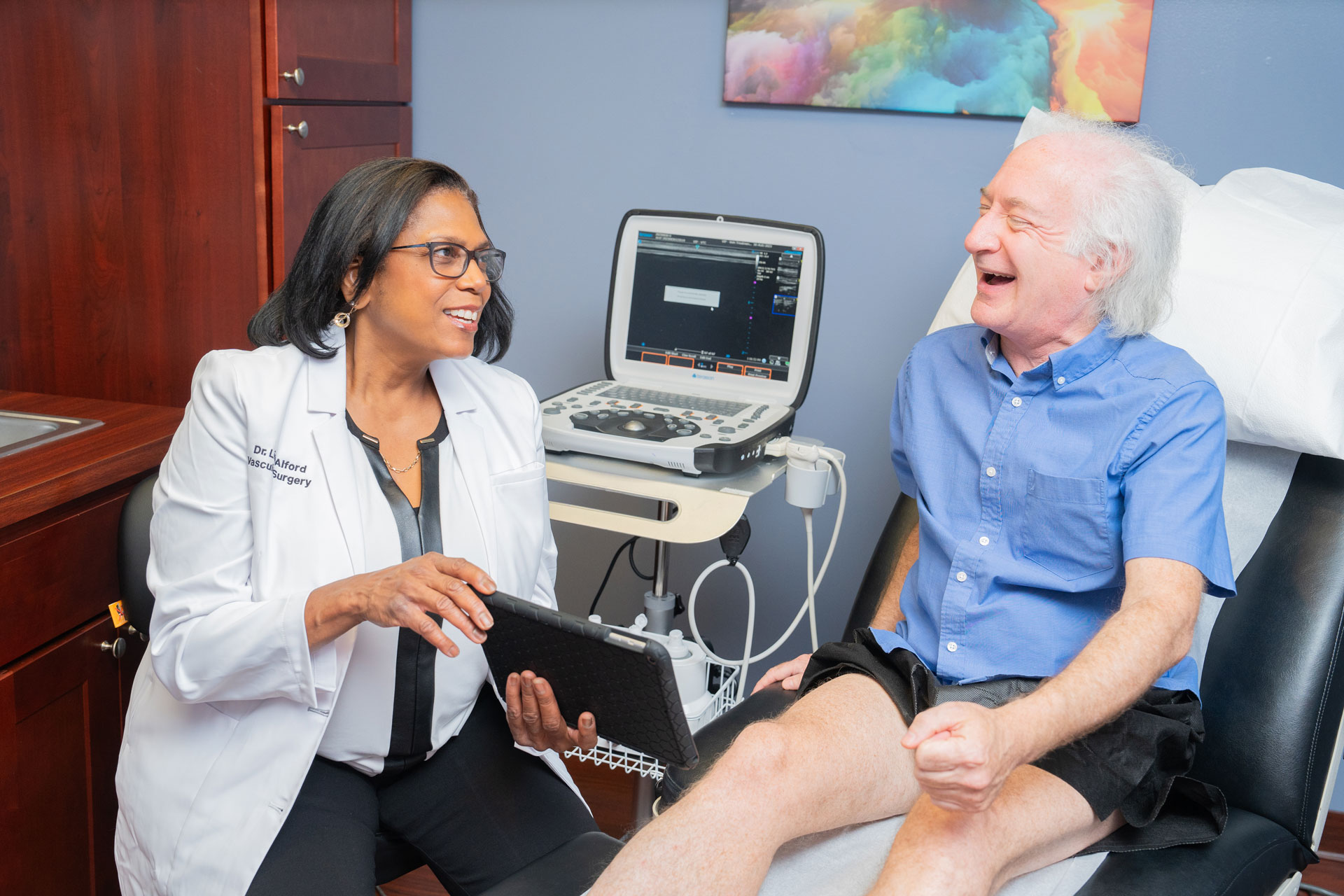
Vein Treatment Clinic is a group of state-of-the-art vein clinics led by board-certified vein doctors dedicated to helping you achieve and maintain optimal vascular health. If you have the signs and symptoms of vein disease, such as leg heaviness, restless legs, or leg pain, especially at the end of the day or after long periods of sitting or standing still, please contact us. You can also contact us if you have a high risk of vein problems and want to mitigate your risk.
Our vein doctors will help you achieve optimal vascular health, manage your symptoms, and treat the root cause of your vein conditions. In this guide, we offer tips to help you improve your venous health, prevent vein diseases, and enjoy a life free from vascular complications.
How Does the Venous System Work?
The venous system consists of a network of blood vessels responsible for returning oxygen-depleted blood from the body’s tissues to the heart. The veins carry deoxygenated blood towards the heart. They have thinner walls and less muscular support compared to arteries, as they don’t need to withstand the high pressure generated by the heart’s contractions.
The veins contain one-way flaps called valves that allow smooth blood flow to the heart. They allow blood to flow towards the heart but close to prevent it from flowing backward. The dysfunction of these valves can lead to chronic venous insufficiency, causing blood to pool in the leg veins. Over time, the continued accumulation of blood in leg veins leads to vascular dilation and the eventual formation of spider veins and varicose veins.
Are you interested in getting more information about your condition or a treatment?
Fill the form below to start!
What Are Common Vein Conditions?
Spider Veins
Spider veins, medically known as telangiectasia, are small, dilated blood vessels near the surface of the skin. They appear as thin, red, or purple lines that often resemble spider webs or tree branches. Unlike varicose veins, spider veins are not inherently harmful and don’t cause significant discomfort. However, they can be a cosmetic concern for many individuals. Furthermore, even though spider veins aren’t directly dangerous, they can often be symptomatic of a dangerous underlying condition: chronic venous insufficiency.
Varicose Veins
Varicose veins are enlarged, twisted veins that commonly occur in the legs. Varicose veins often look like a dense mass of twisted, tangled, and knotted ropes underneath the skin. They result from weakened or damaged vein valves that hinder blood flow back to the heart, causing blood to pool in the veins. Varicose veins can appear as swollen, blue, or purple cords beneath the skin’s surface and often cause discomfort, pain, and leg heaviness.
Chronic Venous Insufficiency (CVI)
Chronic venous insufficiency (CVI) is a medical condition that arises when the veins in the legs are unable to efficiently return blood to the heart. Typically, healthy veins have one-way valves that prevent blood from flowing backward. In CVI, these valves become weakened or damaged, causing blood to pool in the legs. Over time, the continued accumulation of blood in leg veins leads to increased pressure and vascular dilation. This leads to symptoms such as leg swelling, pain, aching, and skin changes, including ulcers.
Deep Vein Thrombosis (DVT)
Deep vein thrombosis (DVT) is a medical condition characterized by the formation of blood clots (thrombi) in deep veins, typically in the legs or pelvis. These clots can obstruct blood flow, causing pain, swelling, and warmth in the affected area. DVT is a serious condition as the clots can dislodge and travel to the lungs, causing a potentially life-threatening condition known as pulmonary embolism. DVT can also occur as a result of untreated chronic venous insufficiency and varicose veins, so prompt diagnosis and treatment are crucial.
What Are the Signs & Symptoms of Venous Issues?
Venous issues can manifest through various signs and symptoms, which may include:
- Visible veins that appear enlarged, twisted, or discolored (varicose veins)
- Leg pain, aching, or discomfort, especially after prolonged standing or sitting
- Swelling in the legs or ankles
- Skin changes, such as redness, itching, or dryness
- Formation of ulcers, particularly around the ankles (venous ulcers)
- A feeling of heaviness or fatigue in the legs
- Cramping or muscle spasms, often occurring at night
- Restless leg syndrome characterized by an irresistible urge to move the legs
- Skin discoloration, especially around the ankles
- A sensation of warmth or heat in the affected area
- Formation of spider veins, which are small, thin, and red or purple in appearance
- Pain or tenderness in the area where a blood clot is present (deep vein thrombosis)
- Shortness of breath, chest pain, and coughing up blood (symptoms of pulmonary embolism)
How Can I Improve Venous Health and Prevent Varicose Veins and Vein Disease?
Improving venous health involves taking proactive steps to support the proper functioning of your veins, maintain healthy circulation, and reduce the risk of varicose veins and vein diseases. While there are no guaranteed ways to prevent vein diseases, implementing certain lifestyle changes can significantly reduce your susceptibility to venous issues. These changes promote better blood flow and alleviate factors that contribute to vein disease, ultimately enhancing your overall well-being. Below, we offer effective strategies to help you improve your venous health and reduce the risk of varicose veins and other vein-related problems.
Tip #1. Stay Physically Active
Engaging in regular physical activity is one of the most effective ways to maintain healthy veins and overall vascular health. Exercise has several positive effects on your venous system:
- Helps blood flow more efficiently through your veins, reducing the risk of blood pooling
- Strengthens the walls of your veins, making them more resilient and less likely to malfunction
- Calf muscles can push blood more effectively to the heart, alleviating the symptoms of CVI
- Maintaining a healthy weight can help prevent obesity, a significant risk factor for CVI
To improve your venous health, aim for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity aerobic activity per week. Activities such as walking, cycling, swimming, and dancing are excellent choices. Additionally, incorporating resistance training to build muscle can also support your venous system.
Tip #2. Elevate Your Legs
Elevating your legs periodically throughout the day can relieve pressure on your veins and help prevent blood from pooling in your lower extremities. When you elevate your legs above heart level, gravity assists in returning blood to the heart. For effective leg elevation, lie down on your back with your legs propped up on pillows or cushions. You should keep your legs elevated for 15-30 minutes. This reduces the risk of swelling and discomfort associated with venous issues and prevents blood from pooling in leg veins.
Consider elevating your legs in the following situations:
- After long periods of standing or sitting
- During breaks at work or home
- When you experience leg fatigue or discomfort
Tip #3. Wear Compression Stockings
Compression stockings are specially designed garments that apply controlled pressure to your legs, promoting healthy blood flow and reducing the risk of vein problems. Wearing compression stockings can help:
- Reduce leg swelling and discomfort
- Prevent the progression of varicose veins
- Minimize the risk of DVT during long flights or periods of immobility
- Alleviate symptoms of CVI, such as pain and skin changes
Consult our vein doctors to determine the appropriate compression level and size for your specific needs. There are different compression levels, and the choice depends on the severity of your venous issues. Wearing an overly loose compression stocking will be ineffective, and an overly tight stocking may cause pain and potentially worsen the condition.
Tip #4. Maintain a Healthy Diet
A balanced diet plays a crucial role in maintaining venous health. Nutrient-rich foods can support the strength and elasticity of your veins. Incorporate the following foods into your diet for optimal venous health:
- Antioxidant-rich fruits and vegetables to protect your veins from inflammation
- A high-fiber diet to promote regular bowel movements and reduce the risk of constipation
- Fatty fish like salmon have anti-inflammatory properties that benefit overall vascular health
- Drink plenty of water to keep your blood thinner and less likely to clot
Tip #5. Stay Hydrated
Adequate hydration is vital for healthy veins. Proper hydration ensures that your blood remains at an optimal consistency. Dehydration can make your blood thicker and more prone to clotting, increasing the risk of venous issues. Aim to drink at least eight glasses (64 ounces) of water per day or more if you’re physically active or in hot weather. Pay attention to your body’s signals for thirst and drink water regularly throughout the day.
Tip #6. Avoid Prolonged Sitting and Standing
Sitting or standing in one position for extended periods can hamper blood circulation in your legs. Incorporate movement and breaks into your routine to improve venous health. Follow these tips to avoid prolonged sitting and standing:
- At work, stand up and walk around for a few minutes every hour
- Use a standing desk or sit-stand workstation if possible
- On long flights or road trips, get up and stretch your legs regularly
- While standing, shift your weight from one leg to the other
- Wear comfortable, supportive shoes
- Use anti-fatigue mats if you stand for extended periods in one location
Tip #7. Avoid Crossing Your Legs
Crossing your legs at the knees when sitting for extended periods can impede blood flow and contribute to venous problems. Over time, this habit can increase the risk of developing varicose veins and exacerbate existing ones. Maintain proper sitting posture by keeping your feet flat on the floor and your knees at a 90-degree angle. If you find it challenging to avoid leg crossing, consider using a footrest to elevate your feet slightly.
Tip #8. Manage Your Weight
Maintaining a healthy weight is essential for venous health, as obesity is a significant risk factor for varicose veins and CVI. Carrying excess weight places added pressure on your veins, especially in the lower extremities. This can lead to weakened vein walls and the development of varicose veins. If you’re overweight, consider these strategies to manage your weight:
- Adopt a balanced, calorie-controlled diet.
- Incorporate regular physical activity into your routine
- Seek support from a healthcare professional or a registered dietitian
Tip #9. Wear Appropriate Footwear
The shoes you wear can significantly affect your venous health. Choosing the right footwear can promote healthy circulation and prevent venous issues. Look for shoes with these features:
- Adequate arch support to maintain proper foot alignment and reduce strain on leg veins
- Low heel height as high heels can strain the calf muscles and impede blood flow
- Comfortable fit as overly tight shoes can constrict blood flow
If you have a job that requires prolonged standing, consider wearing compression socks or stockings in addition to appropriate footwear to provide extra support for your veins.
Tip #10. Elevate Your Bed
Elevating the foot of your bed by a few inches can promote healthy blood circulation while you sleep. By elevating your legs while sleeping, you encourage blood to flow back toward the heart, reducing the risk of blood pooling in your lower extremities. You can achieve bed elevation by using bed risers, which are readily available at most home supply stores. Place them under the bedposts at the foot of your bed to create a gentle incline.
Tip #11. Manage Stress
Chronic stress can negatively impact your overall health, including your venous health. Finding effective stress management techniques is essential for preventing vein diseases. Stress can contribute to venous issues in several ways:
- Stress can lead to overeating and lack of exercise, which can exacerbate vein problems
- It can increase blood pressure, which can strain the veins and lead to varicose veins
- Stress-induced muscle tension can affect blood flow and contribute to discomfort in the legs
To manage stress effectively, consider the following techniques:
- Deep breathing exercises
- Yoga or meditation
- Regular physical activity
- Seeking support from a therapist or counselor
- Finding hobbies and activities that relax and rejuvenate you
Tip #12. Avoid Tight Clothing
Wearing tight clothing, especially around the waist, groin, or legs, can impede blood flow and contribute to vein problems. Tight clothing that compresses your waist or groin area can constrict blood vessels and hinder venous circulation. This can increase the risk of developing varicose veins or exacerbate existing ones. Opt for loose-fitting clothing that allows for proper circulation. If your occupation or personal preference requires tight clothing, consider taking breaks to stretch and move around regularly to promote healthy blood flow.
Tip #13. Elevate Your Feet During Pregnancy
Pregnancy places additional strain on your venous system due to increased blood volume and hormonal changes. During pregnancy, the growing uterus can put pressure on the veins in your pelvis and lower extremities, increasing the risk of varicose veins. Elevating your feet can help alleviate discomfort and reduce the risk of varicose veins. The following are some tips to help you regularly elevate your feet during pregnancy:
- Lie on your left side with your legs propped up on pillows to reduce pressure on the inferior vena cava (a large vein that returns blood to the heart)
- Avoid sitting or standing for extended periods
- Perform ankle exercises to help improve circulation
- Consider wearing maternity compression stockings if recommended by your doctor
Tip #14. Quit Smoking
Smoking is a significant risk factor for venous disease and should be avoided to protect your vascular health. Smoking contributes to venous issues by:
- Increasing the risk of blood clot formation due to the effects of nicotine
- Damaging blood vessels, making them more susceptible to inflammation and clot formation
- Reducing the oxygen-carrying capacity of the blood, which can lead to tissue damage
Tip #15. Limit Alcohol Consumption
Excessive alcohol consumption can negatively affect venous health. It’s important to consume alcohol in moderation to protect your veins. If you choose to drink alcohol, do so in moderation. The Centers for Disease Control and Prevention (CDC) defines moderate drinking as up to one drink per day for women and up to two drinks per day for men. Alcohol can negatively contribute to venous issues by:
- Expanding blood vessels and increasing the pressure within them
- Reducing the efficiency of blood circulation
- Impairing muscle function, making it harder for veins to push blood upward
Tip #16. Regularly Check Your Legs for Changes
Monitoring your legs for any unusual changes can help you catch potential venous issues early, allowing for timely intervention. Regularly inspect your legs for the following changes:
- Swelling, especially in one leg
- Skin discoloration or redness
- Visible veins that appear enlarged or twisted
- Ulcers or open sores on the legs or ankles
- Pain, heaviness, or aching in the legs
If you notice any concerning changes in your legs, consult our vein doctors promptly. Our vein doctors will examine your leg veins, discuss your symptoms, and administer ultrasound tests to determine if you have venous insufficiency. Early detection and treatment can prevent the progression of vein diseases.
Tip #17. Get Regular Check-Ups
Regular medical check-ups are essential for monitoring your overall health, including your venous health. If you have a high risk of vein conditions due to genetics, obesity, or other factors, you should also get regular check-ups from a vein doctor. During routine check-ups, your vein doctor can:
- Assess your risk factors for venous issues
- Perform physical exams to check for signs of vein disease
- Recommend appropriate screenings, such as ultrasound, if necessary
- Provide guidance on maintaining venous health
Venous Health & Wellness FAQs
Can I still exercise if I have varicose veins?
Yes, you can exercise if you have varicose veins. In fact, regular physical activity can help alleviate symptoms and prevent further progression. Low-impact exercises like walking, swimming, and cycling are particularly beneficial. Avoid high-impact activities that may strain your veins. Consult our vein doctors to determine a suitable exercise routine based on the severity of your varicose veins.
Are there any supplements that can improve venous health?
There is no guaranteed supplement that can cure vein diseases. Online sources often peddle unproven claims that horse chestnut, apple cider vinegar, witch hazel, or certain vitamin supplements can treat spider veins or improve vascular health, but these claims should be viewed with skepticism. Most of these claims are unproven and provide little to no real benefits.
At best, some of these solutions may temporarily improve symptoms. Please consult our vein doctors to discuss reliable, effective methods to improve venous health.
Can I wear high heels if I have varicose veins?
While it’s generally recommended to avoid high heels if you have varicose veins, occasional use is usually acceptable. High heels can strain your calf muscles and impede blood flow, exacerbating vein problems. Opt for shoes with lower heels and proper arch support for everyday wear, reserving high heels for special occasions.
Is there a link between pregnancy and varicose veins?
Yes, pregnancy is a common risk factor for varicose veins. During pregnancy, the growing uterus places increased pressure on the veins in the pelvic and lower extremities. Hormonal changes can also contribute to vein relaxation and dilation. To minimize the risk, pregnant individuals should wear compression stockings, avoid prolonged standing or sitting, and consider elevating their legs regularly.
Can obesity worsen venous health?
Yes, obesity is a significant risk factor for venous issues, including varicose veins and chronic venous insufficiency (CVI). Excess weight places additional pressure on your veins, particularly those in the lower extremities. This can lead to weakened vein walls and increased strain on vein valves, contributing to venous problems. Maintaining a healthy weight through diet and exercise is crucial for preventing and managing venous conditions.
Is there a difference between spider veins and varicose veins in terms of treatment?
Yes, there is a difference in the treatment approaches for spider veins and varicose veins. Spider veins, which are typically smaller and closer to the skin’s surface, can often be treated with non-invasive methods like sclerotherapy. Varicose veins may require more advanced treatments, such as ambulatory phlebectomy or Varithena.
Furthermore, spider veins are not always caused by underlying venous insufficiency, but varicose veins are almost always indicative of vein disease. As such, depending on whether you have underlying vein disease, you may also need minimally invasive vein treatments like endovenous laser ablation and radiofrequency ablation. These treatments target the diseased saphenous vein responsible for your vein problems, following which superficial varicose veins and spider veins can be treated.
Can I still enjoy outdoor activities with venous issues?
Yes, you can continue to enjoy outdoor activities with venous issues, provided you take certain precautions. Engage in activities that promote circulation, like hiking or walking, and wear appropriate footwear and compression stockings if necessary. Stay well-hydrated and avoid prolonged periods of standing or sitting. Consult our vein doctors for recommendations based on your specific condition.
Is it possible to have vein diseases without visible symptoms?
Yes, it is possible to have vein diseases without visible symptoms, especially in the early stages. Conditions like chronic venous insufficiency (CVI) may manifest initially with subtle symptoms or discomfort that goes unnoticed. It’s essential to be aware of risk factors and family history and undergo regular check-ups with our vein doctors to detect vein diseases in their early stages. Timely intervention can prevent the progression of these conditions.
Can vein diseases affect men as well, or are they predominantly a women’s issue?
Vein diseases can affect both men and women, although they are more commonly associated with women since the progesterone hormone, which is more prominent in women, can often relax the vein valves, increasing the risk of vein disease. Furthermore, pregnancy and other hormonal changes can also increase the risk of varicose veins. However, men can also develop varicose veins, spider veins, and other vein conditions, particularly if they have risk factors such as genetics, obesity, or a sedentary lifestyle.
Is it safe to treat varicose veins during pregnancy?
Treating varicose veins during pregnancy is generally not recommended due to the increased risk of complications. However, there are conservative measures you can take to alleviate symptoms, such as wearing compression stockings, elevating your legs, and staying active. Consult your vein doctor for guidance and to discuss potential treatment options after childbirth.
Schedule Your Consultation Today
Vein Treatment Clinic is your trusted partner in improving venous health. Our team of board-certified vein doctors is committed to providing personalized evaluations and recommendations to enhance your vascular well-being. Our vein doctors discuss your symptoms and understand your medical history and risk factors to offer personalized lifestyle recommendations to improve overall vascular health and wellness.
We also conduct thorough assessments to determine if you have underlying vein disease and design personalized treatment plans. At Vein Treatment Clinic, we understand the importance of accessible care. That’s why we offer free insurance verifications to help you navigate your treatments seamlessly. With state-of-the-art offices in New York, Long Island, New Jersey, California, and Maryland, you can easily find a location near you for a consultation.