Spider Veins vs. Varicose Veins: Understanding the Key Differences
If you’ve ever noticed unsightly veins on your legs, you might have wondered whether they are spider veins or varicose veins. While both conditions involve visible veins and often occur in the legs, they are distinct in several ways. However, regardless of whether you have spider veins or varicose veins, you should definitely consult a vein doctor because they can both be symptomatic of a more dangerous underlying condition known as chronic venous insufficiency.
The Vein Treatment Clinic is led by talented, highly skilled, board-certified vein doctors who specialize in diagnosing and treating the root causes of spider veins and varicose veins. Instead of simply removing existing veins, our vein doctors treat the root cause and the damaged vein responsible for the problems, thus reducing the risk of future vein problems. Furthermore, our vein doctors only offer minimally invasive vein treatments that involve no downtime.
You can find our vein treatment clinics in New York City, Long Island, New Jersey, Maryland, and California. Please schedule an appointment at your nearest vein clinic today. And if you’re interested in learning more about your condition, please continue reading. In this guide, we explore the differences between spider veins and varicose veins, helping you understand the causes, symptoms, and minimally invasive treatment options for each.
Anatomy and Appearance
Spider Veins
Spider veins, also known as telangiectasias, are tiny, thin veins that appear near the surface of the skin. They often resemble a spider’s web or tree branches, hence the name. Spider veins can be red, blue, or purple in color and are typically less than one millimeter in diameter. They are commonly found on the face and legs but can appear on other parts of the body as well.
Varicose Veins
In contrast, varicose veins are larger and more pronounced. They can appear twisted, swollen, and rope-like in texture. Varicose veins tend to bulge out from the skin’s surface and are typically blue or dark purple. These veins are usually larger than three millimeters in diameter and are most commonly found in the legs, particularly the thighs, calves, and ankles.
Are you interested in getting more information about your condition or a treatment?
Fill the form below to start!

Underlying Causes
Spider Veins
Spider veins usually develop due to the dilation of small blood vessels near the skin’s surface. Although the exact cause can vary, risk factors often include genetics, hormonal changes (such as pregnancy or hormonal therapy), prolonged sitting or standing, and sun exposure. They are generally a cosmetic concern rather than a medical issue.
However, while spider veins aren’t inherently dangerous, they can often be symptomatic of chronic venous insufficiency. This is a condition wherein the vein valves responsible for effective one-way blood flow to the heart malfunction, allowing blood to pool in the leg veins. In some cases, spider veins can be caused by venous insufficiency, and if so, it can be dangerous.
Varicose Veins
Varicose veins almost always result from chronic venous insufficiency and a malfunction in the larger veins located deeper within the legs. This typically involves the valves within the veins, which allow blood to flow in one direction—upward toward the heart. When these valves become weak or damaged, blood can pool in the veins, causing them to become enlarged.
Family history, obesity, pregnancy, and prolonged standing or sitting can contribute to varicose vein development. However, chronic venous insufficiency remains the true root cause of varicose veins. Since venous insufficiency is a chronic condition, varicose veins only worsen with time. If you have varicose veins, you must consult vein doctors without delay.
Symptoms
Spider Veins
Spider veins are primarily a cosmetic issue and often do not cause any physical symptoms. However, some individuals with spider veins may experience mild itching, burning, or aching sensations in the affected area. If your spider veins are caused by underlying vein disease, you may also experience leg heaviness, leg swelling, restless leg syndrome, frequent leg cramps, and, over time, more serious complications like venous ulcers and deep vein thrombosis.
Varicose Veins
Varicose veins are more likely to cause discomfort and physical symptoms. Common symptoms of varicose veins include aching or throbbing pain, a feeling of heaviness in the legs, swelling (edema), cramps, and skin changes like redness or inflammation. Furthermore, since varicose veins are almost always caused by vein disease, untreated varicose veins can lead to leg ulcers, skin infections, and blood clots in the deep veins (deep vein thrombosis).
Diagnosis
Spider Veins
Diagnosing spider veins is typically straightforward and based on a visual examination by a vein doctor. The vein doctor can examine your leg veins and identify spider veins. However, since spider veins are often symptomatic of venous insufficiency, the vein doctor may recommend a duplex ultrasound scan to visualize the blood flow in your leg veins, which helps them identify vein disease. This is a perfectly safe, non-invasive test.
Varicose Veins
Diagnosing varicose veins may involve a physical examination, but additional tests like ultrasound imaging are often necessary to assess the severity of the condition. Furthermore, duplex ultrasound can help identify valve dysfunction and chronic venous insufficiency. Identifying the root cause of varicose veins is essential because treating varicose veins without addressing underlying vein disease can lead to a high risk of recurrence.
Treatment Options
Spider Veins
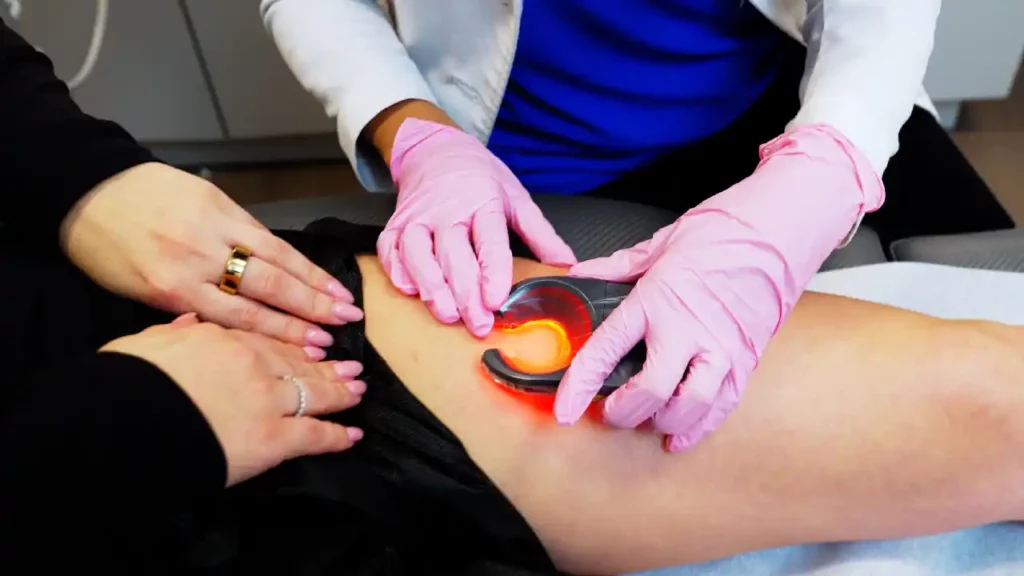
Spider veins are generally treated for cosmetic reasons. If you also have underlying chronic venous insufficiency, your vein doctor may perform treatments like endovenous laser ablation, radiofrequency ablation, or VenaSeal before spider vein treatment. However, if you don’t have vein disease, the vein doctor will only perform a sclerotherapy.
Sclerotherapy is a medical procedure that treats spider veins and smaller varicose veins. It involves injecting a special solution directly into the affected vein. This solution, typically a saline solution or a chemical irritant, causes irritation and inflammation within the vein’s lining. As a result, the vein seals shut and gradually fades from view. Over time, the body absorbs the treated vein, rerouting blood through healthier veins and restoring circulation while diminishing the appearance of the unsightly spider or varicose veins.
Varicose Veins
Varicose veins may require more comprehensive treatment, especially if they cause discomfort or complications. Furthermore, since varicose veins are often caused by underlying vein disease, the vein doctor may first address the root cause before removing the superficial varicose veins from the skin’s surface. The varicose vein treatment options include:
- Endovenous Laser Ablation: EVLA is a minimally invasive procedure used to treat varicose veins. It involves using laser energy delivered through a thin fiber-optic catheter. The catheter is inserted into the affected vein, and the laser is activated. The laser energy generates heat, which causes the vein’s walls to contract and eventually collapse. Over time, the body absorbs the damaged vein, rerouting blood flow through healthier vessels.
- Radiofrequency Ablation: RFA is another minimally invasive treatment for varicose veins. A catheter is inserted into the affected vein, similar to EVLA. However, instead of laser energy, RFA utilizes radiofrequency energy to heat the vein walls. The heat generated by the radiofrequency energy causes the vein to collapse and seal shut. Like EVLA, RFA triggers the body’s natural process of absorbing and rerouting blood flow away from the treated vein.
- Ambulatory Phlebectomy: Ambulatory phlebectomy is a surgical technique used to remove varicose veins close to the skin’s surface. The procedure begins with the administration of local anesthesia to numb the area. Small incisions, typically less than 1/8 inch in size, are made over the varicose veins. A special hook or forceps is then used to grasp and gently remove the damaged vein segments through these tiny incisions. Ambulatory phlebectomy is particularly effective for surface varicose veins and can provide immediate relief.
Spider Veins & Varicose Veins FAQs
Can spider veins turn into varicose veins?
No, spider veins and varicose veins are two distinct conditions. While they share some risk factors and may coexist, spider veins do not necessarily progress into varicose veins.
Can I prevent spider veins and varicose veins if they run in my family?
While genetics play a role in both conditions, you can still reduce your risk by following preventive measures such as maintaining a healthy lifestyle, staying active, and wearing appropriate clothing or compression stockings.
Is there any way to completely prevent varicose veins?
Complete prevention may not be possible, especially if you have a genetic predisposition. However, following preventive measures can reduce your risk and delay their onset.
Schedule Your Consultation Today
Understanding the differences between spider veins and varicose veins is crucial for proper diagnosis and treatment. If you suspect you have either condition, it’s essential to consult a vein doctor for a thorough evaluation and appropriate guidance on treatment and prevention. By taking proactive steps and seeking professional help, you can maintain healthy legs.
At Vein Treatment Clinic, our team of board-certified vein doctors is dedicated to providing you with the most effective and minimally invasive treatments available. Our expert vein specialists start by conducting thorough assessments to accurately diagnose your condition. From there, they develop personalized treatment plans tailored to your unique needs. Whether you require sclerotherapy, endovenous laser ablation, radiofrequency ablation, or another state-of-the-art procedure, our team is committed to helping you achieve the best results.
To make the process even more convenient, we offer free insurance verifications to help you understand your coverage. With state-of-the-art offices in New York, Long Island, New Jersey, California, and Maryland, we’re here to ensure that you receive top-notch vein care. Schedule your consultation today to improve vascular health.