Endovenous Laser Ablation vs. Radiofrequency Ablation: A Comprehensive Comparison
If you’re one of the millions of people who suffer from varicose veins, you may have heard about two popular minimally invasive vein treatments: Endovenous Laser Ablation (EVLA) and Radiofrequency Ablation (RFA). These procedures have revolutionized the management of varicose veins, offering less pain and a quicker recovery compared to traditional surgical options like vein ligation and vein stripping. However, you may be wondering which is right for you.
The Vein Treatment Clinic is led by board-certified vein doctors specializing in cutting-edge minimally invasive treatments for varicose veins and venous insufficiency. Our vein doctors carefully examine your leg veins, review your medical history, and diagnose the root cause of your vein problems using advanced duplex ultrasound tests. Our vein doctors help you select the most appropriate vein treatment for your specific needs, whether that’s EVLA, RFA, or other minimally invasive vein treatments, like VenaSeal, ClariVein, or ambulatory phlebectomy.
In this article, we compare Endovenous Laser Ablation and Radiofrequency Ablation to help you make an informed choice for your varicose veins treatment.
Mechanism of Action
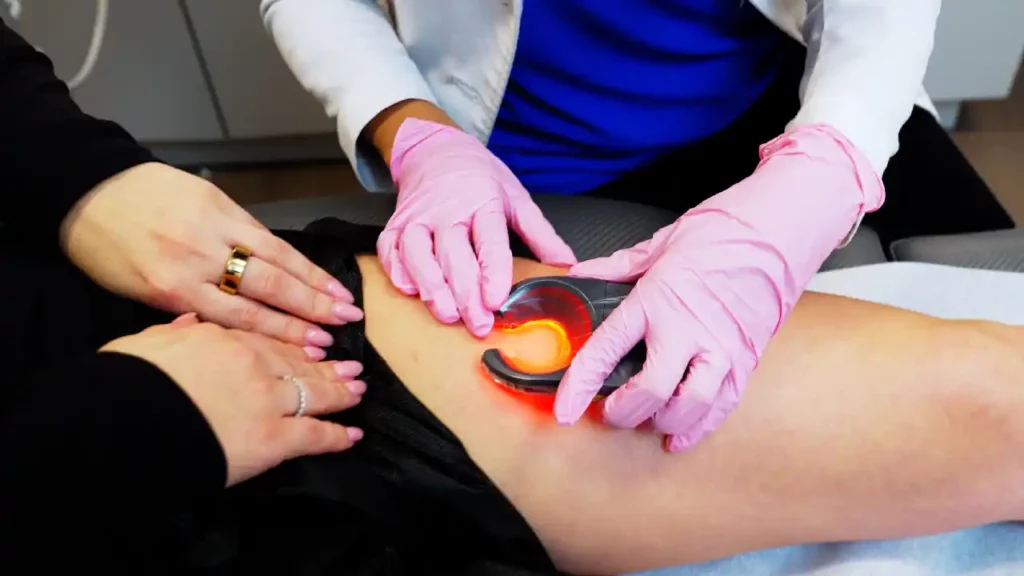
Endovenous Laser Ablation, also known as endovenous laser therapy (EVLT), uses laser energy to treat varicose veins. During the procedure, a laser fiber is inserted into the affected vein through a tiny incision. The laser emits high-energy light waves that heat and close off the problematic vein. This redirects blood flow to healthier veins.
Radiofrequency Ablation, on the other hand, uses radiofrequency energy to treat varicose veins. A catheter with a radiofrequency electrode tip is inserted into the diseased vein. Once positioned, the electrode delivers radiofrequency energy to heat and collapse the vein, allowing for the rerouting of blood to healthier veins and alleviating the symptoms of vein disease.
Are you interested in getting more information about your condition or a treatment?
Fill the form below to start!

Effectiveness
When it comes to effectiveness, both EVLA and RFA are highly successful in treating varicose veins. Studies have shown that both procedures have similar long-term success rates in closing off problematic veins, with success rates exceeding 90% in most cases.
Procedure Duration
EVLA typically takes around 30 to 45 minutes per leg, making it a relatively quick procedure. RFA is also a relatively quick procedure, with an average duration of 30 to 45 minutes per leg.
Anesthesia
EVLA is usually performed under local anesthesia. This means that you will be awake during the procedure, but your leg will be numbed to minimize discomfort. RFA is also performed under local anesthesia, just like EVLA. Both procedures ensure optimal patient comfort.
Pain and Discomfort
Patients experience minimal pain and discomfort during and after EVLA. Some may report a mild burning or tingling sensation as the laser energy is delivered, but this is well-tolerated. Similarly, RFA is associated with minimal pain and discomfort. Patients may feel a sensation of warmth or pressure, and, in some cases, it might be slightly more comfortable than EVLA.
Recovery Time
Most patients can resume normal activities immediately after EVLA and RFA — both are lunchtime procedures that involve no downtime. However, in both cases, compression stockings are recommended for a week or more to aid in healing and reduce swelling, and strenuous workouts and heavy lifting should be avoided for a few days.
Side Effects
EVLA and RFA are generally associated with few side effects. Some patients may experience mild bruising, swelling, or skin discoloration at the treatment site. These side effects are usually temporary and resolve within a few weeks. In rare cases, patients may develop small, tender lumps at the treatment site, which usually resolve on their own.
Cost
The cost of varicose vein treatment can vary depending on factors like geographic location, the severity of your condition, and your insurance plan. In general, both EVLA and RFA tend to be comparable in cost, and both are covered by most insurance providers when deemed medically necessary. Please consult our vein doctors and request free insurance verification for a quote.
Long-Term Results
Both EVLA and RFA have demonstrated excellent long-term results in the treatment of varicose veins. Furthermore, both procedures can treat underlying chronic venous insufficiency, the root cause of most vein problems, thus minimizing the risk of recurrence. New varicose veins can also develop due to genetic predisposition, lifestyle factors, or other issues. Therefore, regular follow-ups and lifestyle modifications are necessary to reduce the risk of recurrence.
Other Minimally Invasive Vein Treatments
VenaSeal
VenaSeal is a minimally invasive treatment for varicose veins that uses a medical adhesive to close off diseased veins. This innovative procedure, also known as cyanoacrylate closure, involves the application of a specialized medical glue into the affected vein. The adhesive rapidly polymerizes, sealing the vein shut permanently. Over time, the body naturally absorbs the sealed vein, rerouting blood through healthier vessels. VenaSeal offers a less painful alternative to traditional surgery and causes minimal discomfort.
ClariVein
ClariVein is a minimally invasive treatment for varicose veins that combines mechanical and chemical approaches to close off problematic veins. During the procedure, a specialized catheter with a rotating tip is inserted into the vein. As the catheter spins, it damages the vein’s inner lining. Simultaneously, a liquid chemical called sclerosant is infused directly into the vein. This combination disrupts the vein’s function, causing it to collapse and eventually be absorbed by the body. ClariVein can treat venous insufficiency and varicose veins.
Varithena
Varithena is a medical foam used to treat varicose veins through a process known as ultrasound-guided foam sclerotherapy. This minimally invasive procedure involves injecting Varithena foam directly into the affected veins. The foam displaces the blood within the vein and irritates its inner lining. This irritation triggers the vein to close and eventually be absorbed by the body. Varithena effectively reduces the symptoms associated with varicose veins and is especially suited for treating larger and more complex vein networks.
Ambulatory Phlebectomy
Ambulatory phlebectomy is a surgical technique used to remove superficial varicose veins near the skin’s surface. During the procedure, small incisions are made over the varicose veins, and a hook-like instrument is inserted to gently extract the affected vein segments. The incisions are typically so small that sutures are not required. Ambulatory phlebectomy is particularly effective for treating visible, bulging varicose veins and is often performed alongside other minimally invasive treatments for comprehensive vein care.
Other Vein Treatment FAQs
How long does the recovery period typically last for both EVLA and RFA procedures?
Both EVLA and RFA procedures offer relatively short recovery times. Most patients can resume their regular activities within a day or two after the treatment. However, it’s essential to follow post-procedure care instructions, which may include wearing compression stockings, to optimize healing and reduce swelling.
Are there any significant differences in cost between EVLA and RFA?
The cost of varicose vein treatment, including EVLA and RFA, can vary based on several factors, including your location and the severity of your condition. Generally, these two procedures are comparable in cost. It’s advisable to consult your vein doctor to determine the specific costs involved in your case.
Can VenaSeal, ClariVein, or Varithena be used in combination with EVLA or RFA?
Yes, in some cases, VenaSeal, ClariVein, or Varithena may be used in combination with EVLA or RFA to address different aspects of varicose vein treatment. Your vein doctor will assess your condition and recommend the most suitable combination of treatments for optimal results.
Is there a risk of varicose vein recurrence after undergoing EVLA or RFA?
While both EVLA and RFA have high success rates in closing off varicose veins, new varicose veins can develop over time due to various factors, including genetics and lifestyle. Regular follow-up appointments with your vein doctor and lifestyle modifications are essential to monitor your condition and prevent recurrence.
How long does an ambulatory phlebectomy procedure typically take?
The duration of an ambulatory phlebectomy procedure depends on the number and size of varicose veins being removed. Generally, it takes about 30 minutes to an hour to complete. It’s considered a relatively quick surgical option for addressing visible varicose veins.
Is ambulatory phlebectomy a suitable treatment for all types of varicose veins?
Ambulatory phlebectomy is particularly effective for treating superficial varicose veins near the skin’s surface. However, it may not be the best option for deep-seated or more complex vein networks, and it can’t treat chronic venous insufficiency, the root cause of most vein problems. That’s why it’s often performed after EVLA and RFA to remove visible veins.
Choosing the Right Vein Treatment
The success of EVLA and RFA procedures relies heavily on the skill and experience of the vein doctor performing them. Your choice should be influenced by factors such as the size of your varicose veins, your personal comfort level, and the expertise of your chosen vein doctor. Whether you opt for EVLA or RFA, the goal is the same – to alleviate the discomfort and concerns associated with varicose veins and improve your overall quality of life.
It’s essential to choose a board-certified vein doctor with expertise in minimally invasive vein treatments to ensure the best possible outcome. The board-certified vein doctors at Vein Treatment Clinic consider all possible factors when recommending vein treatments, including the root cause of your vein problems, your medical history, and more. Please schedule an appointment at your nearest vein treatment clinic to explore your vein treatment options.