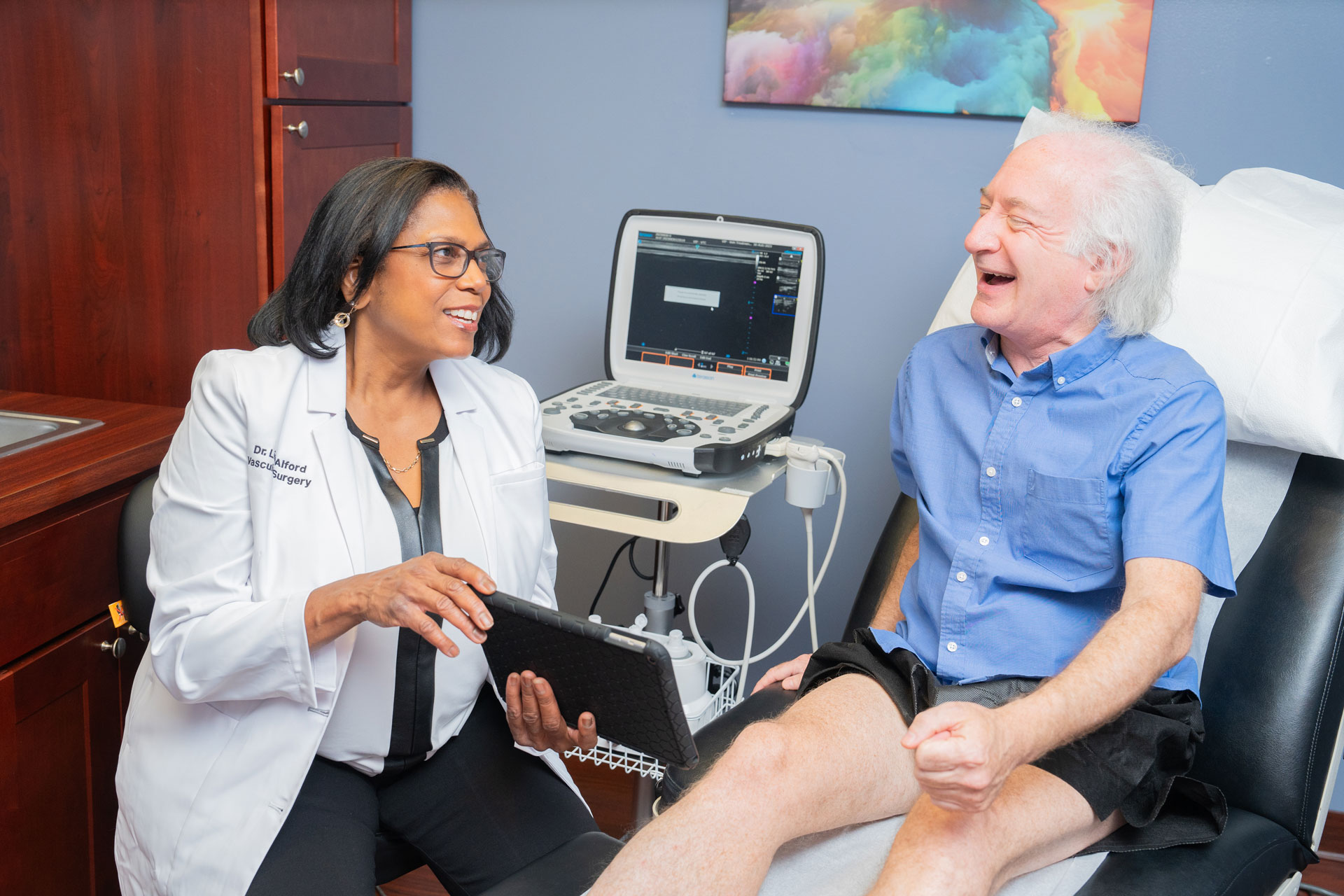
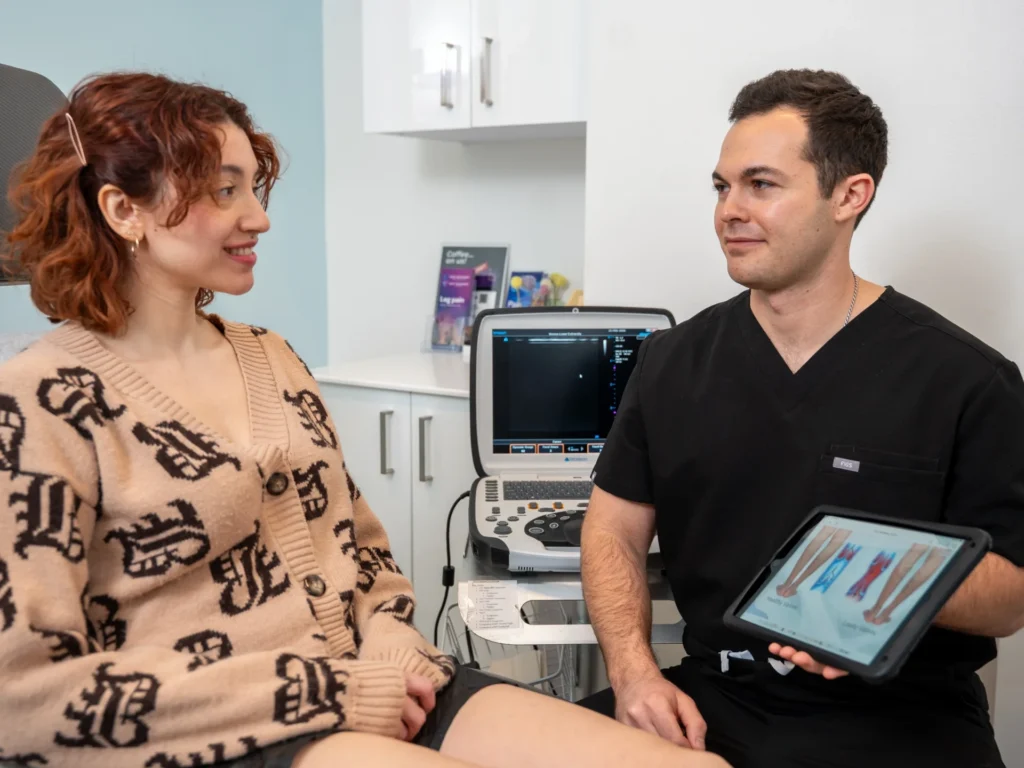
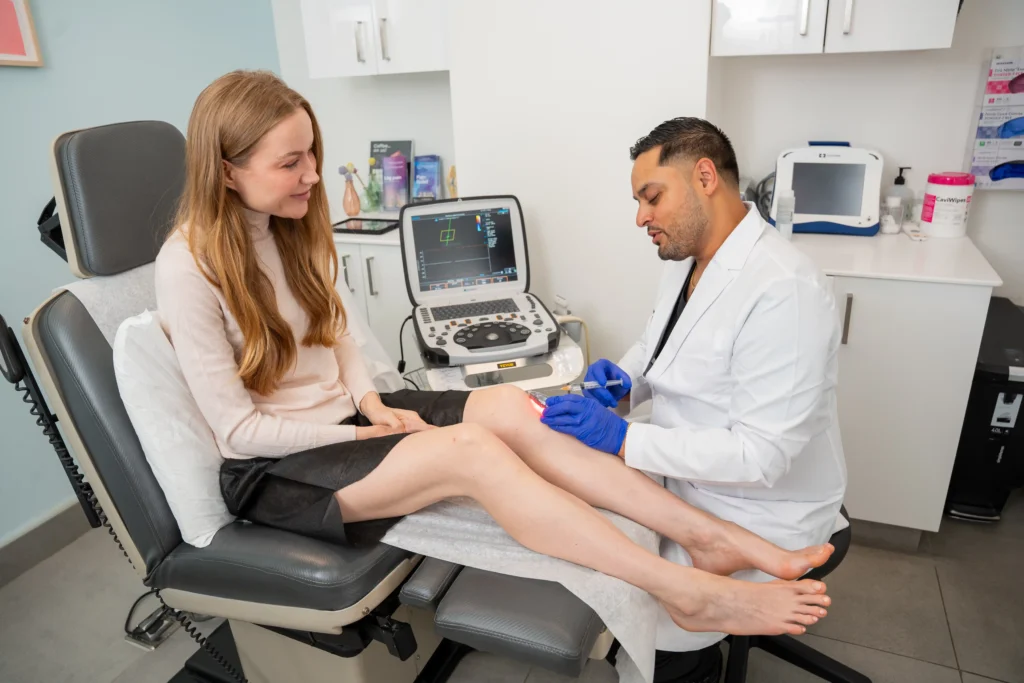
The Link Between CVI and Skin Conditions: What You Need to Know
Chronic venous insufficiency (CVI) is a circulatory disorder that affects millions of people worldwide, yet few people understand it. In fact, it’s one of the most underdiagnosed conditions because its initial warning signs and symptoms, such as leg heaviness, leg pain, and leg cramps, can be misattributed to aging, exhaustion, pregnancy, or other factors. Yet, chronic venous insufficiency is a dangerous condition, and, left untreated, it can eventually lead to severe complications like leg ulcers and deep vein thrombosis.
Chronic venous insufficiency occurs when the vein valves responsible for ensuring smooth one-way blood flow to the heart collapse or malfunction. This causes blood to flow backward and accumulate in the leg veins, eventually leading to spider veins, varicose veins, and other problems. While it primarily involves the veins of the lower extremities, many are unaware of the impact it can have on the skin. This article explores the link between CVI and skin conditions.
The Impact of CVI on Skin Health
Skin Discoloration
One of the most noticeable effects of CVI on the skin is skin discoloration. Due to the accumulation of blood in the lower extremities, the skin can take on a reddish-brown or purplish hue. This is often referred to as “stasis dermatitis” and is a common early sign of CVI. Stasis dermatitis is a result of the increased pressure in the veins, which can lead to leakage of red blood cells and hemosiderin into the surrounding tissues. This can cause a noticeable change in the color of your skin, particularly around the ankles and lower legs.
Itching and Dryness
Many individuals with CVI experience persistent itching and dryness of the skin. This can be attributed to the inflammation and irritation caused by the pooling of blood and the presence of hemosiderin in the tissues. The constant itchiness can be quite uncomfortable and may lead to scratching, which can further damage the skin and increase the risk of infection.
Venous Stasis Ulcers
Venous stasis ulcers are one of the more severe skin complications associated with CVI. These are open sores that typically develop around the ankles or lower legs. Venous stasis ulcers occur when the increased pressure in the veins causes damage to the skin and underlying tissues, leading to the breakdown of the skin’s integrity. These ulcers can be painful and challenging to heal. They often require specialized wound care and may take several weeks or even months to close completely. If left untreated, venous stasis ulcers can become infected and cause more significant health issues.
Cellulitis
Another skin condition that can be linked to CVI is cellulitis. Cellulitis is a bacterial skin infection that can develop when bacteria enter the body through breaks or cracks in the skin. The constant itching, scratching, and skin damage associated with CVI can create an entry point for bacteria, increasing the risk of cellulitis. Cellulitis typically presents with redness, warmth, swelling, and tenderness in the affected area. It is a serious condition that requires prompt medical attention and treatment with antibiotics.
Are you interested in getting more information about your condition or a treatment?
Fill the form below to start!

Managing Skin Conditions in CVI
Compression Therapy
Compression therapy can also help prevent and alleviate skin complications. Compression stockings or bandages are worn to apply pressure to the legs, helping to improve blood flow and reduce swelling. This can help prevent skin discoloration and venous stasis ulcers. It’s essential to consult our vein doctors for proper fitting and guidance on using compression stockings.
Skin Hydration
Keeping the skin well-hydrated is essential for individuals with CVI. Moisturizing creams or ointments can help combat the dryness and itching associated with CVI. However, it’s crucial to choose moisturizers that are suitable for sensitive and compromised skin, as fragranced or harsh products may exacerbate skin issues.
Elevation
Elevating the legs whenever possible is another effective way to manage CVI and reduce the risk of skin complications. Elevating the legs above heart level can help promote better blood flow, leveraging gravity to direct excess blood to the heart, thus reducing swelling and pressure in the veins. This can aid in preventing venous stasis ulcers and skin discoloration.
Proper Wound Care
If venous stasis ulcers or other skin issues develop, it’s crucial to seek medical attention. Proper wound care is essential to prevent infection and promote healing. Vein doctors can provide guidance on wound dressings, cleaning, and topical medications to support healing.
Infection Prevention
To reduce the risk of cellulitis and other skin infections, individuals with CVI should be diligent about keeping their skin clean and avoiding unnecessary scratching. Any signs of infection, such as redness, warmth, or swelling, should be reported to your vein doctor immediately.
Treating Chronic Venous Insufficiency
Lifestyle changes can undoubtedly play a crucial role in preventing chronic venous insufficiency (CVI) from worsening. These changes often include maintaining a healthy weight, engaging in regular physical activity, and wearing compression stockings. However, it’s important to note that lifestyle modifications primarily manage the symptoms and slow down the progression of CVI rather than treat its root cause. To effectively address CVI and prevent associated skin conditions, minimally invasive vein treatments are necessary. The board-certified vein doctors at Vein Treatment Clinic specialize in diagnosing and treating the root cause of vein problems using the latest and safest minimally invasive vein treatments.
Endovenous Laser Ablation
Endovenous laser ablation (EVLA) is a highly effective minimally invasive procedure used to treat CVI. During EVLA, a thin laser fiber is inserted into the affected vein through a small incision. The laser emits precise energy that causes the vein’s walls to collapse and seal shut. This redirects blood flow to healthier veins, alleviating the pressure and symptoms associated with CVI. Over time, the treated vein is absorbed by the body, improving both blood circulation and the appearance of the skin.
Radiofrequency Ablation
Radiofrequency ablation (RFA) is another minimally invasive technique used to treat CVI. A specialized catheter is inserted into the affected vein. The catheter delivers radiofrequency energy, which generates heat and causes the vein to contract and collapse. Like EVLA, this procedure redirects blood flow to healthier veins and facilitates the body’s natural healing process. RFA is a safe and effective way to address CVI and related skin conditions.
ClariVein
ClariVein is a unique and minimally invasive technique for treating CVI. During this procedure, a rotating wire is inserted into the affected vein while a special sclerosing solution is dispersed. The wire’s rotation ensures even distribution of the solution, which irritates the vein’s walls and causes them to collapse and close. ClariVein is a well-tolerated and effective option for addressing CVI and its associated varicose veins.
Ambulatory Phlebectomy
Ambulatory phlebectomy is a minimally invasive surgical technique used to remove superficial varicose veins. During this procedure, tiny incisions are made near the affected veins, and a hook-like instrument is used to extract the veins through these incisions. Ambulatory phlebectomy is used in conjunction with other minimally invasive treatments to improve both the appearance of the skin and the overall vascular health.
Sclerotherapy
Sclerotherapy is a versatile, minimally invasive procedure used to treat both small varicose veins and spider veins. During sclerotherapy, a sclerosant solution is injected directly into the affected veins, causing them to collapse and eventually fade away. This treatment is highly effective for addressing cosmetic concerns associated with CVI and is often used alongside other treatments for comprehensive vein care.
Consult Our Vein Doctors for CVI Treatment
Chronic venous insufficiency (CVI) is not solely a vascular issue but also has a significant impact on skin health. Skin conditions such as discoloration, itching, venous stasis ulcers, and cellulitis are closely linked to CVI and require attention as part of the overall management of the condition. While lifestyle changes can alleviate some of the symptoms, the only way to treat CVI and prevent complications is through minimally invasive vein treatments.
Vein Treatment Clinic is led by board-certified vein doctors specializing in cutting-edge, minimally invasive spider vein and varicose vein treatments. Our vein doctors curate personalized treatment plans to address your symptoms and improve overall vascular health. Please schedule an appointment to explore your vein treatment options.