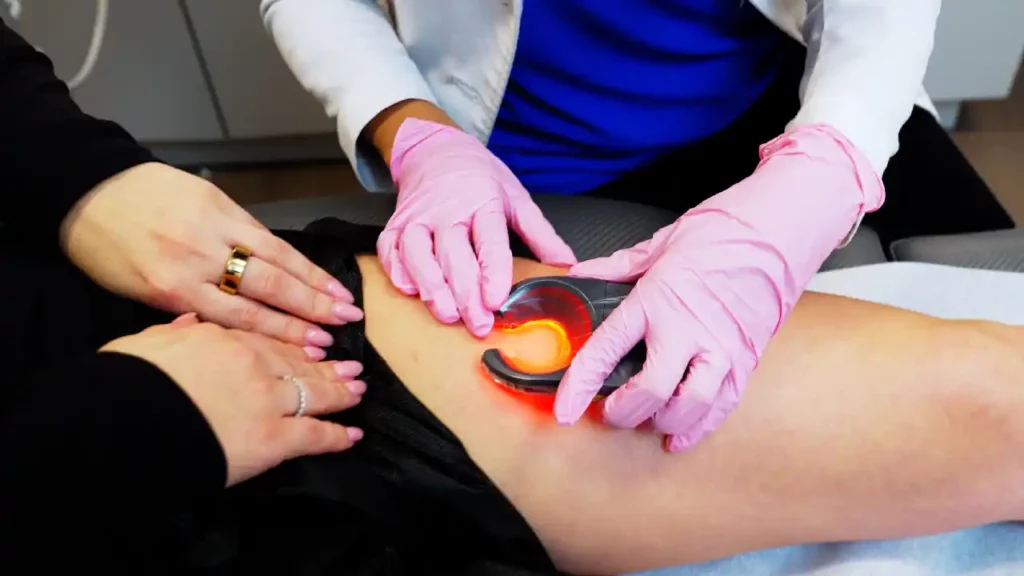
Can Exercise Help Manage Chronic Venous Insufficiency (CVI)?
Chronic venous insufficiency (CVI), a common condition that affects millions of people worldwide, occurs when the veins in the legs fail to efficiently return blood to the heart, leading to a range of uncomfortable and potentially serious symptoms. If you’re among those who suffer from CVI, you may be wondering how exercise can play a role in managing this condition. In this article, we explore the link between exercise and CVI, offering you insights and tips to manage your condition and prevent the symptoms from worsening.
Please note that exercise can only alleviate some of the discomfort and prevent venous insufficiency from worsening. However, venous insufficiency is caused by damaged vein valves, and the only true solution is medical intervention. Vein Treatment Clinic is led by board-certified vein doctors who offer minimally invasive treatments to close the diseased vein and reroute the accumulated blood into healthier leg veins, restoring optimal blood flow to the heart. That’s the only real way to treat chronic venous insufficiency.
If you have the signs and symptoms of vein disease, please schedule an appointment with our board-certified vein doctors. In the meantime, please follow the tips mentioned in this article to exercise, improve vascular health, and prevent venous insufficiency from worsening.
What Is Chronic Venous Insufficiency (CVI)?
CVI occurs when the valves in your leg veins do not function properly, causing blood to flow backward and pool in the veins. This can lead to a range of symptoms, including:
- Swelling in the legs and ankles
- Pain or aching in the affected leg
- Heavy or tired-feeling legs
- Itchy or dry skin on the legs
- Skin discoloration, typically around the ankles
- Leg ulcers, in severe cases
CVI can result from various factors, including genetics, obesity, pregnancy, a sedentary lifestyle, and prolonged periods of standing or sitting. Managing CVI is crucial to prevent complications and improve your overall quality of life.
Are you interested in getting more information about your condition or a treatment?
Fill the form below to start!
Exercise and CVI: The Connection
Regular exercise can be a valuable tool in managing CVI. It offers several benefits that directly address the underlying causes and symptoms of this condition.
- Improved Blood Circulation: Engaging in physical activity promotes the contraction of leg muscles, which helps push blood upward, against gravity, towards the heart. This enhanced circulation reduces the pooling of blood in the veins and eases the strain on the veins.
- Strengthening of Leg Muscles: Exercising regularly strengthens the muscles in your legs, which play a vital role in assisting the veins to return blood efficiently. Stronger leg muscles can provide better support to the venous valves, preventing blood from flowing backward and reducing the risk of venous insufficiency.
- Weight Management: Obesity is a known risk factor for CVI. Exercise can help you achieve and maintain a healthy weight, reducing the pressure on your veins. Losing excess weight can alleviate symptoms and decrease the risk of CVI worsening.
- Reduction in Inflammation: Chronic inflammation can exacerbate the symptoms of CVI. Exercise has been shown to reduce inflammation in the body, which can have a positive impact on the vascular system and alleviate some of the symptoms of venous insufficiency.
Exercise Recommendations for CVI
Now that you understand the benefits of exercise for CVI, you may be wondering what types of exercise are most effective and safe for you. Here are some recommendations:
- Low-Impact Aerobic Activities: Engage in low-impact aerobic exercises like walking, cycling, or swimming. These activities promote blood circulation without putting excessive strain on your leg veins. Start slowly and gradually increase the intensity and duration of your workouts.
- Leg Elevation Exercises: Perform leg elevation exercises to help reduce swelling and improve blood flow in the legs. Lie flat on your back and elevate your legs above heart level for 15-20 minutes a few times a day.
- Strength Training: Incorporate strength training exercises that target the muscles in your legs, such as leg lifts, squats, and calf raises. Building muscle strength can support your veins and improve blood flow to the heart, thus alleviating the symptoms of CVI.
Other Lifestyle Recommendations for CVI
In addition to exercise, you can also implement a few other lifestyle changes to improve blood circulation and alleviate the symptoms of CVI. These include:
- Healthy Diet: Maintain a well-balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Adequate fiber intake can help prevent constipation, which can worsen CVI.
- Hydration: Stay well-hydrated to support overall vascular health and prevent dehydration-related issues that can exacerbate CVI symptoms.
- Avoid Prolonged Sitting or Standing: If your job or lifestyle involves extended periods of sitting or standing, take regular breaks to walk and stretch your legs.
- Compression Garments: Consider wearing compression stockings or garments. These can provide external support to your veins and improve blood flow.
- Leg Elevation: Elevate your legs above heart level when resting, especially after prolonged periods of sitting or standing, to reduce swelling and improve venous return.
- Smoking Cessation: If you smoke, quitting is highly recommended, as smoking can exacerbate CVI symptoms and increase the risk of vascular complications.
- Avoid Tight Clothing: Refrain from wearing tight clothing, especially around the waist and groin area, as it can restrict blood flow and exacerbate CVI symptoms.
Common Questions About Exercise & CVI
Can exercise cure CVI?
Exercise cannot cure CVI, as it is often a chronic condition. However, regular physical activity can significantly improve the symptoms and slow the progression of the disease.
How often should I exercise to manage CVI?
Aim for at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity aerobic exercise per week, as recommended by the American Heart Association. You can break this down into shorter sessions throughout the week.
Is it safe to exercise if I have CVI-related leg ulcers?
Exercise can still be safe and beneficial if you have leg ulcers due to CVI. However, it’s crucial to consult your vein doctor for guidance on exercise modifications and wound care.
Are there any exercises I should avoid with CVI?
High-impact exercises, such as jumping, may increase the risk of exacerbating CVI symptoms and should be avoided. Additionally, exercises that put excessive pressure on the legs, such as heavy lifting, may not be suitable.
Can exercise worsen CVI?
Exercise, when performed correctly and in consultation with your vein doctor, should not worsen CVI. However, it’s essential to choose appropriate exercises and listen to your body. If you experience increased pain or discomfort during or after exercise, stop and rest.
Can exercise prevent the development of CVI?
Regular exercise can reduce the risk of developing CVI, particularly if you are at risk due to genetics or lifestyle factors. Maintaining a healthy weight and an active lifestyle can be preventive measures against venous insufficiency.
Can I do exercises at home to manage CVI?
Yes, many exercises that benefit CVI can be done at home. Leg lifts, ankle pumps, and seated bicycle exercises are just a few examples you can incorporate into your daily routine.
Minimally Invasive Treatments for CVI
Lifestyle changes and exercise can alleviate symptoms and prevent venous insufficiency from worsening, but they can’t treat the root cause of the problem. Vein Treatment Clinic offers the latest and safest minimally invasive treatments for CVI, including:
- Endovenous Laser Ablation: EVLA is a minimally invasive procedure that uses laser energy to close off faulty veins. A thin laser fiber is inserted into the affected vein, and laser energy is applied to heat and seal the vein shut. EVLA is typically performed on larger varicose veins and offers excellent results with minimal scarring or discomfort.
- Radiofrequency Ablation: Similar to EVLA, radiofrequency ablation uses thermal energy to close off diseased veins. A catheter with a radiofrequency electrode is inserted into the vein, and radiofrequency energy is applied to heat and collapse the vein walls. Radiofrequency ablation is effective for treating both varicose veins and venous insufficiency.
- VenaSeal: VenaSeal is a newer, minimally invasive treatment that uses a medical adhesive to seal malfunctioning veins. A small catheter is inserted into the vein, and the adhesive is injected to seal the vein shut. VenaSeal is a quick and virtually painless procedure, with minimal bruising and a rapid recovery period.
- Ambulatory Phlebectomy: Ambulatory phlebectomy is a surgical procedure that removes surface varicose veins through tiny incisions. It is often performed alongside other minimally invasive treatments to remove visible varicose veins.
- Sclerotherapy: Sclerotherapy is a common treatment for spider veins and smaller varicose veins. A special solution is injected into the affected veins, causing them to collapse and eventually be reabsorbed by the body. Multiple sessions may be required for optimal results.
These minimally invasive treatments offer several advantages for CVI management, including shorter recovery times, minimal scarring, and reduced discomfort compared to traditional surgical options. The choice of treatment depends on the severity of your CVI, the size and location of the affected veins, and your vein doctor’s recommendations. Please schedule a consultation with our board-certified vein doctors to determine the most suitable treatment plan for your specific condition.