Chronic Venous Insufficiency (CVI): A Comprehensive Guide
Chronic venous insufficiency (CVI) is a vascular condition that affects millions of individuals worldwide. This chronic condition occurs when the veins in the legs struggle to efficiently return blood to the heart, leading to various uncomfortable symptoms and potential complications. Even though venous insufficiency is an extremely common, chronic condition, it’s highly underdiagnosed. That’s because the early signs and symptoms of venous insufficiency are often misattributed to aging, exhaustion, or other factors.
If you experience leg pain, swelling, leg cramps, or restless legs, especially at the end of the day or after long periods of sitting or standing still, you should definitely consult vein doctors. These symptoms are often indicative of underlying vein disease. In this comprehensive guide, we provide all the information you need about chronic venous insufficiency, including its signs and symptoms, causes, risks, and treatment options.
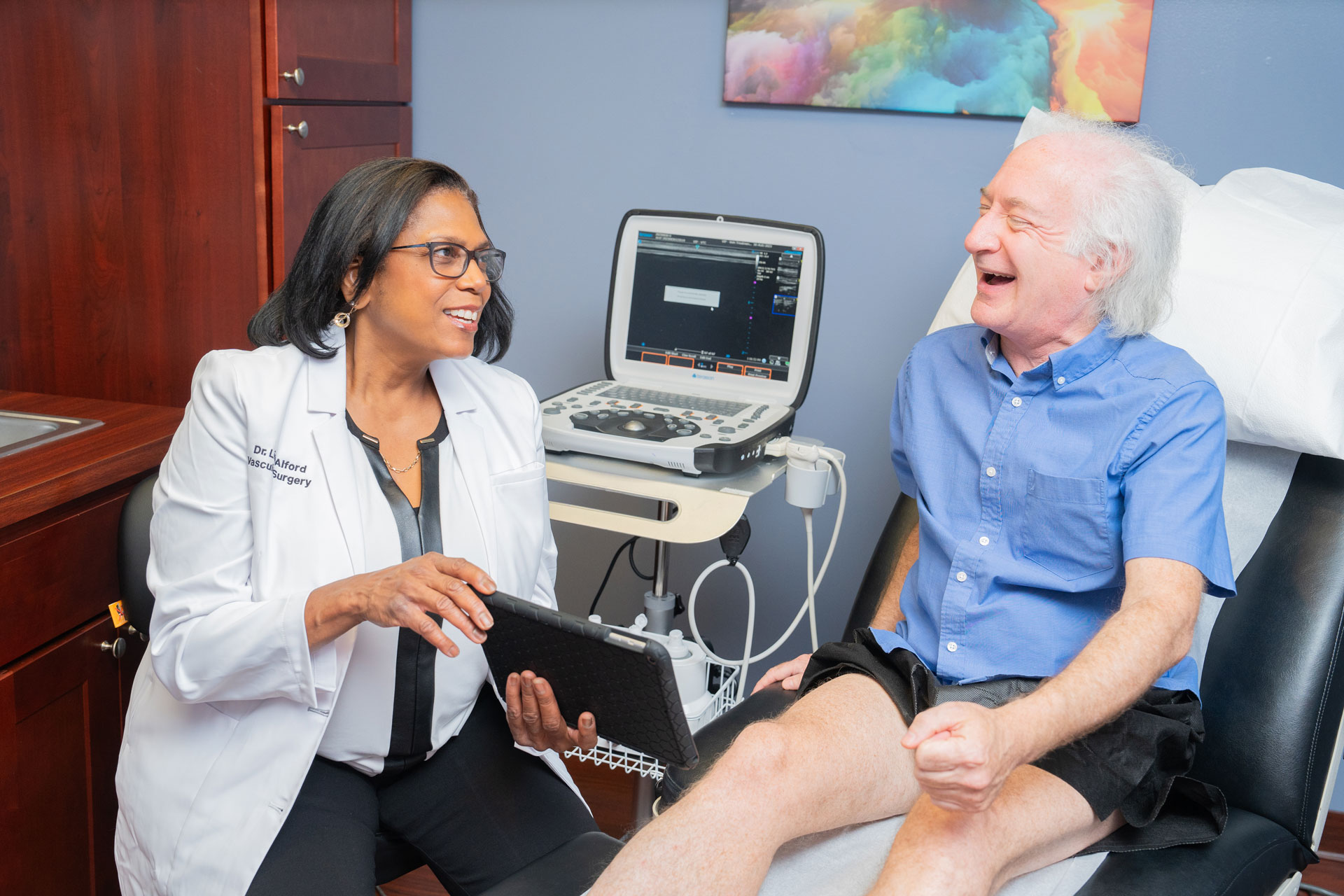
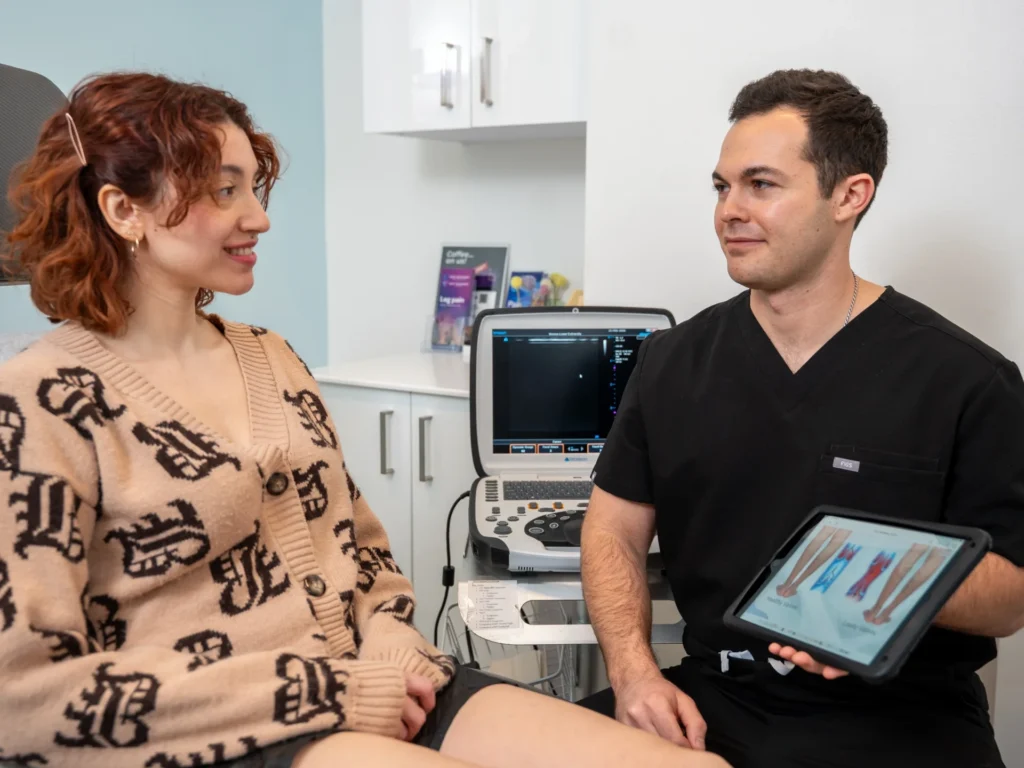
At Vein Treatment Clinic, we offer safe, cutting-edge, minimally invasive treatments for vein disease. Our board-certified vein doctors carefully examine your leg veins, discuss your symptoms, review your medical history, and curate personalized treatment plans to improve your vascular health. We have state-of-the-art offices across the United States, including New York, New Jersey, California, and Maryland. Please schedule an appointment at your nearest vein clinic for a thorough evaluation, diagnosis, and treatment.
What Is Chronic Venous Insufficiency (CVI)?
Chronic Venous Insufficiency (CVI) is a complex vascular disorder that primarily affects the lower extremities, resulting from an impairment in the normal functioning of veins. To understand CVI, you must understand the role of the two main types of blood vessels in the body: arteries and veins. Arteries carry oxygen-rich blood away from the heart to nourish the body’s tissues and organs, while veins are responsible for returning oxygen-depleted blood back to the heart.
In a healthy vascular system, veins rely on a series of one-way valves to facilitate the upward flow of blood against gravity. These valves open to allow blood to move toward the heart and close to prevent backflow. However, in the case of CVI, these valves become damaged or weakened, failing to close properly. As a result, blood begins to pool in the lower limbs rather than efficiently returning to the heart. This leads to increased pressure within the leg veins.

What Are the Risk Factors for CVI?
Chronic venous insufficiency (CVI) occurs when the valves responsible for allowing one-way blood flow to the heart malfunction or collapse. While CVI can affect anyone, certain factors can increase the likelihood of its development. Here are some common risk factors for CVI:
- Age: Over time, the veins and valves in the legs naturally undergo wear and tear. The aging process can lead to a reduction in vein elasticity and the overall integrity of vein walls. As a result, elderly individuals are at a higher risk of developing CVI compared to younger adults.
- Gender: Women are more susceptible to CVI than men, with hormonal factors playing a significant role. Hormonal changes during pregnancy and menopause can weaken vein walls and valves, leading to a higher risk of vein disease.
- Family History: A family history of CVI or varicose veins suggests a genetic predisposition to the condition. If your parents or close relatives have experienced CVI, your vein valves may be more susceptible to weakening or collapsing.
- Obesity: Excess body weight places additional stress on the veins in the legs. This increased pressure can lead to vein valve dysfunction and hinder proper blood flow. Obesity is not only a risk factor for CVI development but can also exacerbate existing CVI symptoms.
- Prolonged Standing or Sitting: Jobs or lifestyles that involve prolonged periods of standing or sitting can contribute to CVI risk. When you stand for extended periods, blood has to work against gravity to return to the heart. Similarly, sitting for long hours can impede healthy blood circulation. Both scenarios can lead to weakened vein valves over time.
- Pregnancy: As the uterus enlarges during pregnancy, it can exert pressure on the pelvic veins, impeding blood flow from the legs. Hormonal changes during pregnancy can also relax vein walls and valves, making them more prone to dysfunction. While CVI symptoms may improve after childbirth, the risk remains higher during pregnancy.
- History of Deep Vein Thrombosis (DVT): A previous episode of DVT, where blood clots form in the deep veins of the legs, can damage vein valves and hinder blood flow. This damage can contribute to the development of CVI or exacerbate existing CVI symptoms.
What Are the Signs & Symptoms of CVI?
Chronic venous insufficiency causes blood to accumulate in the leg veins, leading to increased vascular pressure in the legs and poor blood circulation. Over time, the continued accumulation of blood in leg veins can lead to numerous signs and symptoms, including:
- Leg pain and discomfort
- Aching and cramping sensations in the legs
- Edema or swelling, primarily in the lower legs and ankles
- Visible varicose veins — enlarged, twisted, or bulging veins near the surface of the skin
- Skin changes in the affected area, including darkening or discoloration
- Inflammation or redness of the skin, especially around the ankles
- Itching and burning sensations in the legs
- An irresistible urge to move the legs (restless legs syndrome)
- Development of painful open sores that may be difficult to heal (venous ulcers)
- Spider veins (telangiectasia) — small, red or blue, web-like veins on the skin’s surface
- Fatigue and heaviness in the legs, especially after prolonged periods of standing or sitting
- Leg cramps, particularly during the night
- Skin dryness and scaling in the affected area
- Red, itchy, and inflamed skin, known as venous eczema or stasis dermatitis
- Thicker, hardened skin near the ankles and lower legs (lipodermatosclerosis)
The combination and severity of these symptoms can vary from person to person and may worsen over time if left untreated. If you suspect you may have CVI or are experiencing any of these signs and symptoms, please consult our vein doctors for a comprehensive evaluation.
What Are the Stages of CVI?
Chronic venous insufficiency is categorized into various stages based on the severity of the condition. CVI stages are typically classified as follows:
- Stage 0: There are typically no visible symptoms or signs of CVI. However, underlying venous issues may still be present. Patients in this stage may have underlying venous insufficiency detected through diagnostic tests but do not yet display visible symptoms.
- Stage 1: Visible varicose veins become apparent. These are often unsightly and may cause some discomfort, but they are usually not accompanied by more severe symptoms. Stage 1 CVI primarily involves cosmetic concerns related to the appearance of the legs.
- Stage 2: This is characterized by the onset of symptoms. Patients may experience discomfort, aching, or pain in the legs, particularly after prolonged periods of standing or sitting. Skin changes, such as pigmentation or inflammation, may also become noticeable.
- Stage 3: Patients may experience more pronounced symptoms. Chronic leg swelling becomes more prominent, along with significant pain, skin changes, and the development of venous ulcers. The skin may become discolored and exhibit visible signs of vein disease.
- Stage 4: The most advanced stage of CVI involves severe venous ulceration. Venous ulcers are painful open sores that are challenging to heal without intervention. These ulcers often develop in areas where the skin has been damaged due to long-term venous insufficiency.
How Can I Manage CVI?
The only way to treat chronic venous insufficiency is through minimally invasive vein treatments performed by vein doctors. However, you can implement a few lifestyle changes to alleviate some symptoms and prevent the condition from worsening. Here are some lifestyle changes to manage your venous insufficiency symptoms:
- Wear Compression Stockings: Compression stockings are specially designed to apply gentle pressure on your legs, helping to improve blood flow and prevent swelling. They come in various compression levels, so it’s essential to consult a vein doctor to determine the right level of compression for your condition.
- Stay Active: Regular, low-impact exercises, such as walking, swimming, or cycling, can promote circulation in your legs. Exercise strengthens the calf muscles, which play a crucial role in helping blood flow back to the heart, reducing the symptoms of CVI.
- Elevate Your Legs: Elevating your legs above heart level whenever possible can reduce swelling and discomfort. Lie down and prop your legs up on pillows or cushions to encourage blood flow away from your lower extremities.
- Maintain a Healthy Weight: Excess body weight places added pressure on your leg veins, potentially worsening CVI symptoms. Achieving and maintaining a healthy weight through diet and exercise can alleviate this pressure.
- Avoid Prolonged Sitting or Standing: Prolonged periods of sitting or standing can strain your leg veins. Take short breaks to walk or flex your calf muscles regularly, especially if your job requires extended periods of sitting or standing.
- Stay Hydrated: Proper hydration supports overall vascular health. Drinking enough water helps maintain blood volume, making it easier for your veins to function efficiently.
- Avoid Tight Clothing: Tight clothing, particularly around the waist, groin, or legs, can impede blood flow. Choose loose-fitting garments to prevent constriction and maintain healthy veins.
- Regularly Check Your Legs: Routinely inspect your legs for any new symptoms, changes in skin color, or the appearance of varicose or spider veins. Promptly report any concerns to your vein specialist for evaluation and guidance.
How Is CVI Diagnosed?
At Vein Treatment Clinic, our board-certified vein doctors provide comprehensive care to individuals with vascular conditions. Our approach involves a meticulous diagnostic process that identifies CVI and assesses any associated superficial vein issues, such as spider veins and varicose veins. This allows us to curate a personalized treatment plan tailored to your needs.
Physical Examination
The first step in diagnosing CVI involves a thorough physical examination conducted by our vein specialists. We assess the condition of your legs, paying close attention to any visible signs or symptoms indicative of CVI. Our vein doctors will look for varicose veins, spider veins, changes in skin texture, and areas of swelling or discoloration. A detailed assessment of your medical history, including any family history of venous issues, will also be considered.
Symptom Assessment
Understanding your specific symptoms is a crucial aspect of the diagnostic process. Our vein specialists will engage in a detailed discussion with you to ascertain the nature, duration, and severity of your symptoms. This dialogue helps us gain insight into how CVI is affecting your daily life, whether you’re experiencing pain, swelling, discomfort, or other related issues.
Duplex Ultrasound Tests
To confirm CVI and assess its severity, we often use duplex ultrasound tests. This test provides a clear visual representation of your vein structure and function. During the test, a handheld device is used to transmit high-frequency sound waves into the affected area. These sound waves bounce off the blood cells in your veins, creating images that reveal the direction and speed of blood flow. Duplex ultrasound helps us identify issues such as blood clots, valve dysfunction, or reflux (backward flow of blood) in the veins.
Our board-certified vein doctors analyze the ultrasound results to determine the precise location and extent of vein abnormalities. This information is invaluable in developing a customized treatment plan that addresses your specific CVI-related concerns. At Vein Treatment Clinic, our commitment to accurate diagnosis ensures you receive the most appropriate and effective treatments for your CVI and any associated vein conditions.
What Treatment Options Are Available for CVI?
At Vein Treatment Clinic, we are committed to providing the highest standard of care for individuals with chronic venous insufficiency (CVI) and related vein conditions. Our approach centers on personalized, minimally invasive vein treatments and avoiding surgery. Minimally invasive treatments have emerged as safer and more effective alternatives, offering quicker recovery times and fewer complications than outdated surgical options. In addition to CVI, we also treat the visible signs of venous insufficiency, including varicose veins and spider veins, thus addressing your medical and aesthetic concerns.
Compression Stockings
Compression stockings are specialized garments designed to treat and manage vein diseases like CVI. They work by applying gentle, graduated pressure on the legs, helping to improve blood flow and reduce swelling and discomfort. While compression stockings can prevent the condition from worsening and alleviate some symptoms, they do not treat the underlying cause of CVI. Minimally invasive treatments like endovenous laser ablation and radiofrequency ablation are more effective in addressing CVI at its source.
Endovenous Laser Ablation (EVLA)
Endovenous laser ablation (EVLA) is a minimally invasive procedure used to treat chronic venous insufficiency. During EVLA, a thin laser fiber is inserted into the affected vein through a small incision. Laser energy, typically in the form of diode lasers, is delivered into the vein’s interior. The laser energy causes the vein’s inner wall to heat up and collapse, sealing it shut. This process redirects blood flow to healthier veins, improving overall circulation.
Radiofrequency Ablation (RFA)
Radiofrequency ablation (RFA) involves using radiofrequency energy generated by a specialized catheter to create controlled heat within the affected vein. This heat causes the vein’s collagen fibers to contract and the vein itself to close. Once closed, blood is rerouted to healthier veins, relieving CVI symptoms. RFA is a highly effective treatment option, offering minimal discomfort and a faster recovery compared to traditional surgical methods.
VenaSeal Closure
VenaSeal Closure is a cutting-edge, minimally invasive treatment that involves using a medical adhesive or “vein glue” that is injected into the affected vein using a catheter. The adhesive seals the vein shut, effectively closing it off. Over time, the body naturally absorbs the sealed vein, rerouting blood flow to healthier veins. VenaSeal Closure is virtually painless, requires no anesthesia, and allows for immediate resumption of daily activities.
ClariVein
ClariVein is an innovative treatment for chronic venous insufficiency (CVI) and large, tortuous varicose veins. During the procedure, a specialized catheter with a rotating wire tip is inserted into the affected vein. The catheter agitates and damages the vein’s inner lining while delivering a sclerosing agent, usually in foam form, to seal the vein. This dual-action approach disrupts the vein’s function and encourages it to close off. ClariVein is particularly effective for treating larger varicose veins with irregular shapes.
Varithena
Varithena is a foam sclerotherapy treatment used to address chronic venous insufficiency (CVI) and varicose veins. During the procedure, a foam solution is injected into the affected veins. This foam displaces blood within the vein, causing it to collapse and close off. The injected foam also irritates the vein’s inner lining, promoting inflammation and sealing the vein shut. Over time, the body naturally absorbs the closed vein, redirecting blood flow to healthier vessels. Varithena is effective for treating veins with irregular shapes and sizes.
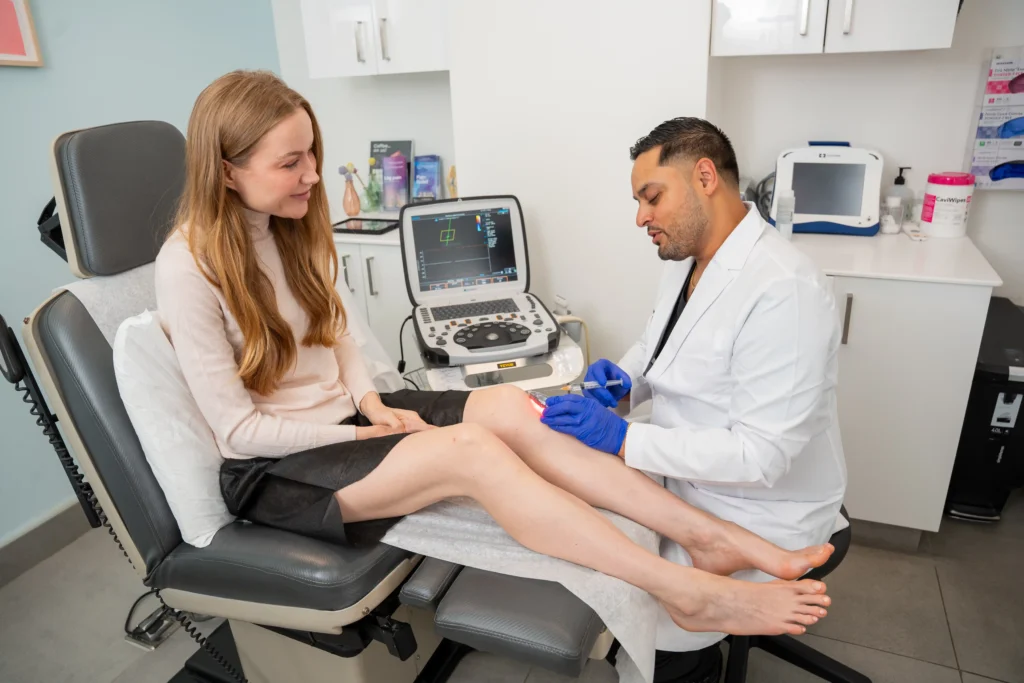
Sclerotherapy
Sclerotherapy is widely used for treating smaller varicose veins and spider veins, common consequences of venous insufficiency. During the procedure, a special solution called a sclerosant is injected directly into the affected veins. The sclerosant irritates the vein’s inner lining, causing it to collapse and stick together. Over time, the sealed vein is absorbed by the body, and blood flow is rerouted through healthier veins. Sclerotherapy is highly effective in improving the appearance of visible veins and alleviating related symptoms.
Ambulatory Phlebectomy
Ambulatory phlebectomy is a surgical procedure used to treat larger varicose veins. During this procedure, small incisions are made in the skin near the affected vein. A special hook-like instrument is used to remove the varicose vein in sections through these incisions. Ambulatory Phlebectomy is effective for larger, bulging varicose veins that may not respond to minimally invasive treatments. While it is more invasive, it provides immediate cosmetic improvement.
What Are the Benefits of Minimally Invasive Vein Treatments?
In the not-so-distant past, the only way to treat venous insufficiency was through complex surgical procedures that involved hospitalization, general anesthesia, large incisions, and considerable downtime. But thanks to recent advances in medicine, we can now treat venous insufficiency using safe, in-office, minimally invasive vein treatments. The following are some of the benefits of minimally invasive treatments for CVI:
- Highly effective in treating CVI and improving circulation
- Patients generally experience less pain and discomfort compared to surgical methods
- Offer faster recovery times, allowing patients to return to normal activities sooner
- Can be performed using local anesthesia, eliminating the need for general anesthesia
- Result in minimal scarring and cosmetic impact
- Associated with a lower risk of complications compared to surgery
- Performed on an outpatient basis, reducing the need for hospital stays
- Can be tailored to each patient’s specific needs, ensuring the best possible outcome
- Often more cost-effective than surgery since there’s no hospitalization
- Lower risk of infections and complications than surgery
What Happens After Minimally Invasive Vein Treatments?
After undergoing minimally invasive vein treatments for CVI, you can expect a relatively smooth recovery. Most people can resume their daily activities immediately. In fact, many of our patients undergo vein treatments during their lunch break and then resume work immediately. You may have to wear compression stockings and avoid strenuous workouts for a few days, but there are no major activity restrictions. Furthermore, post-treatment side effects like swelling, redness, and bruising dissipate over a few days.
After undergoing minimally invasive vein treatments, it’s crucial to adhere to specific aftercare guidelines to optimize recovery and maintain treatment results. These include:
- Your doctor may recommend wearing compression stockings to aid in healing.
- Gentle, regular walking and leg movement can reduce the risk of blood clots.
- Minimize extended periods of sitting or standing to prevent additional strain on your veins.
- If prescribed, take any medications or pain relievers as directed by your physician.
- Proper hydration is essential for overall vascular health.
- To prevent vein dilation, avoid hot baths and saunas for a specified period after treatment.
- Protect treated areas from excessive sun exposure to prevent skin discoloration.
- Elevate your legs when resting to reduce swelling and discomfort.
- Attend all scheduled follow-up appointments to monitor progress and ensure proper healing.
Chronic Venous Insufficiency (CVI) FAQs
What is the main difference between CVI and varicose veins?
CVI is a condition that results from the malfunction of vein valves, leading to poor blood circulation in the legs. Varicose veins, on the other hand, are swollen and twisted veins that often develop as a consequence of CVI. While CVI is the underlying cause, varicose veins are a visible symptom of this condition.
Are there any non-invasive or natural remedies for CVI?
While there is no cure for CVI through non-invasive or natural means, certain lifestyle changes can help manage symptoms. Regular exercise, elevation of the legs, wearing compression stockings, and maintaining a balanced diet can alleviate discomfort and improve blood flow. However, the only way to treat vein disease is through minimally invasive vein treatments.
How long does it take to recover after minimally invasive vein treatments?
Recovery time varies depending on the specific procedure and the individual’s overall health. In general, minimally invasive treatments for CVI offer a quicker recovery compared to traditional surgery. Most patients can return to their regular activities immediately after the procedure. However, it’s crucial to follow your vein specialist’s aftercare guidelines, such as avoiding strenuous workouts and direct sunlight for a few days and wearing compression stockings.
Can CVI lead to more serious health issues?
Yes, CVI can potentially lead to more severe complications if left untreated. It can cause skin changes, such as pigmentation and ulcers, which can become infected. In some cases, CVI may contribute to the development of deep vein thrombosis (DVT), a serious condition involving blood clots in deep veins. Early diagnosis and treatment are essential to prevent these risks.
Can I undergo minimally invasive vein treatments if I have other medical conditions or take medications?
Your vein specialist will conduct a thorough evaluation of your medical history and current health status to determine the most suitable treatment approach. In most cases, minimally invasive treatments are safe for individuals with other medical conditions or those taking medications. However, it’s essential to inform your vein doctor of all your medical conditions and medications to ensure the safest and most effective treatment plan.
Are the results of minimally invasive vein treatments permanent?
Minimally invasive vein treatments can provide long-lasting relief from CVI symptoms, but it’s essential to understand that they may not prevent new veins from becoming problematic in the future. However, the treated veins are typically permanently sealed off, and the symptoms associated with those specific veins should not return.
Can I resume physical activities and exercise after minimally invasive vein treatments?
Most patients can resume physical activities and exercise shortly after minimally invasive vein treatments. In fact, light exercise, such as walking, is encouraged as it can promote circulation and aid in recovery. However, it’s essential to follow your doctor’s recommendations regarding the timing and intensity of exercise, as this may vary depending on your specific treatment.
How often should I have follow-up appointments after vein treatment?
The frequency of follow-ups may vary depending on your specific condition and the treatment you received. In general, your vein specialist will schedule initial follow-ups to monitor your progress and assess the effectiveness of the treatment. After the initial phase, less frequent appointments may be recommended to ensure long-term success.
Schedule Your Consultation Today
If you suspect you may have chronic venous insufficiency (CVI) or are experiencing symptoms such as leg pain, swelling, or visible varicose veins, it’s crucial to seek professional evaluation and treatment. At Vein Treatment Clinic, our board-certified vein specialists are dedicated to providing comprehensive care for CVI and related vein conditions.
Don’t wait for your symptoms to worsen or for potential complications to develop. Schedule your consultation with us today to start your journey toward healthier veins and improved well-being. During your consultation, our vein doctors will conduct a thorough evaluation, discuss your concerns, and recommend a personalized treatment plan. We offer state-of-the-art, minimally invasive vein treatments to ensure optimal safety and convenience.
Vein Treatment Clinic has state-of-the-art offices in New York City, Long Island, New Jersey, California, and Maryland. Please schedule an appointment at your nearest vein clinic today.